High Blood Pressure Risk: Understanding Long-Term Health Implications
This page provides population-level education on high blood pressure risk, long-term health implications, and how clinicians interpret trends and variability over time. It is intended for informational purposes only.


What Is High Blood Pressure?
Blood pressure is a measure of the force exerted by circulating blood against the walls of the arteries. It reflects how hard the heart must work to move blood through the body.
High blood pressure, also known as hypertension, occurs when this force remains elevated over time. It is often asymptomatic, meaning many individuals are unaware of elevated levels.
Because symptoms are usually absent, high blood pressure is commonly identified through routine measurement rather than physical signs.
Why High Blood Pressure Increases Health Risk Over Time
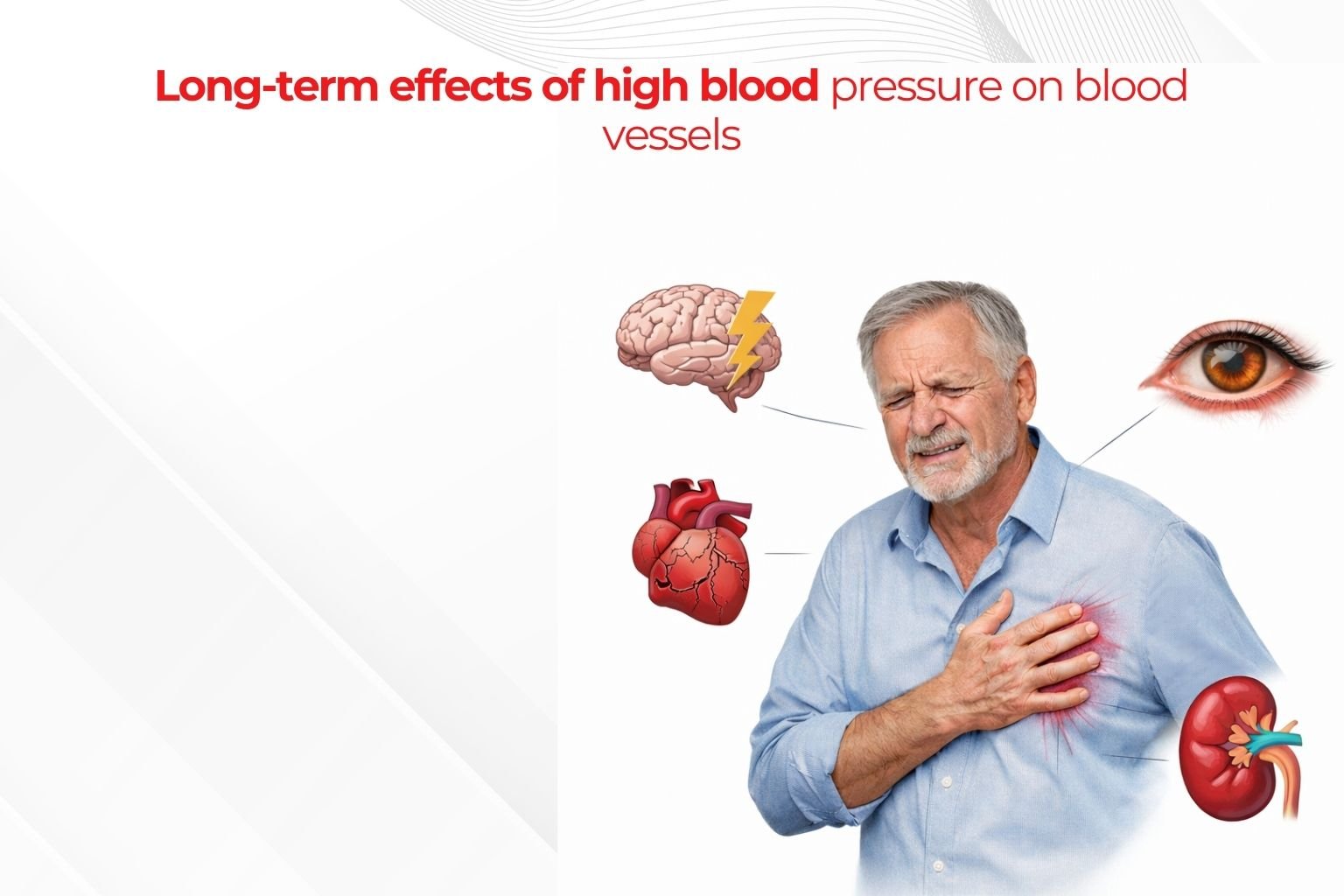
Over time, persistently elevated blood pressure places strain on blood vessel walls. This chronic stress can contribute to changes in vascular structure and function.
Health risk associated with high blood pressure is cumulative. Duration and consistency of elevation often matter more than isolated readings.
Long-term exposure to elevated pressure is associated with increased likelihood of cardiovascular and cerebrovascular conditions, although individual outcomes vary.
Blood Pressure Trends and Variability

Blood pressure naturally fluctuates throughout the day in response to activity, stress, posture, and sleep. These variations are normal and expected.
Some individuals experience higher readings in clinical settings (often called white-coat hypertension), while others may have elevated readings outside the clinic (masked hypertension).
Clinicians often evaluate patterns over time rather than individual readings.
Understanding trends and variability provides more context than isolated measurements.
Factors That Influence Blood Pressure Risk

Blood pressure risk is influenced by a combination of genetic, biological, and environmental factors.
These include age, family history, dietary patterns, physical activity levels, stress, co-existing health conditions, and certain medications.
Risk profiles are individualized and may change over time.
Heart Health Monitoring at Home — What It Can and Cannot Show

Home blood pressure measurements can provide additional data about readings outside the clinical environment. They may help capture variability and patterns.
Home measurements provide data, not diagnoses.
Interpretation of readings requires clinical context, and isolated values should not be used to draw conclusions about health status.
Clinician-Reviewed Hypertension Management Approaches

Hypertension management approaches are determined by clinicians and may include lifestyle modification, medication, monitoring, and follow-up.
Management approaches are individualized and determined by clinicians.
Clinical oversight is central to evaluating risk and guiding care decisions.
When Blood Pressure Risk Warrants Medical Attention

Persistent elevation, significant variability, symptoms when they occur, or a history of cardiovascular conditions may prompt further medical evaluation.
Decisions about evaluation and follow-up are made by healthcare professionals based on individual circumstances.
What This Page Does Not Claim
This page does not recommend treatments, suggest products, compare solutions, imply outcomes, or provide care guidance.
It does not determine eligibility for monitoring or clinical programs.
This content is provided for educational purposes only.
Related Health Topics
Educational content on stroke risk factors and warning signs.
How to Prevent a StrokeAn overview of how clinicians use monitoring data in hypertension care.
Remote Blood Pressure MonitoringLearn how medical-grade devices are defined and evaluated.
High Blood Pressure MonitoringMedical content reviewed by qualified healthcare professionals. References include guidance from the Centers for Disease Control and Prevention (CDC), the American Heart Association (AHA), and the National Institutes of Health (NIH).