Stroke prevention is centered on reducing known risk factors through clinically supported strategies. While no intervention can eliminate risk entirely, early management and consistent medical care can significantly lower the likelihood of stroke.
What Causes Strokes?
A stroke occurs when blood flow to part of the brain is disrupted, depriving brain tissue of oxygen and nutrients. The two primary categories are ischemic strokes, caused by blocked blood vessels, and hemorrhagic strokes, caused by bleeding within or around the brain.
The majority of strokes are associated with modifiable risk factors, including high blood pressure, diabetes, high cholesterol, smoking, atrial fibrillation, sleep disorders such as sleep apnea, obesity, and physical inactivity. Genetic predisposition and age also contribute to risk.
Because stroke is usually the result of long-term vascular damage, prevention focuses on sustained risk reduction rather than short-term interventions.
Stroke prevention is based on probability reduction, not absolute prevention. Individual risk varies and should be assessed by a qualified healthcare professional.
Proven Ways to Reduce Stroke Risk
Blood Pressure Control
Hypertension is the strongest modifiable risk factor for stroke. Maintaining blood pressure within recommended ranges through lifestyle changes and prescribed treatment significantly lowers risk.
Diabetes Management
Poorly controlled blood glucose accelerates vascular damage. Consistent diabetes management reduces long-term injury to blood vessels supplying the brain.
Smoking Cessation
Tobacco use damages the vascular lining and promotes clot formation. Stopping smoking leads to measurable risk reduction over time.
Regular Physical Activity
Moderate, consistent exercise improves circulation, supports metabolic health, and contributes to healthier blood pressure and cholesterol levels.
Medication Adherence
Antihypertensives, statins, antiplatelet agents, and other prescribed therapies are effective only when taken as directed. Inconsistent use increases stroke risk.
Cholesterol Management
Elevated LDL cholesterol contributes to plaque formation and arterial narrowing. Maintaining recommended lipid levels reduces ischemic stroke risk.
Early Stroke Warning Signs Everyone Should Know
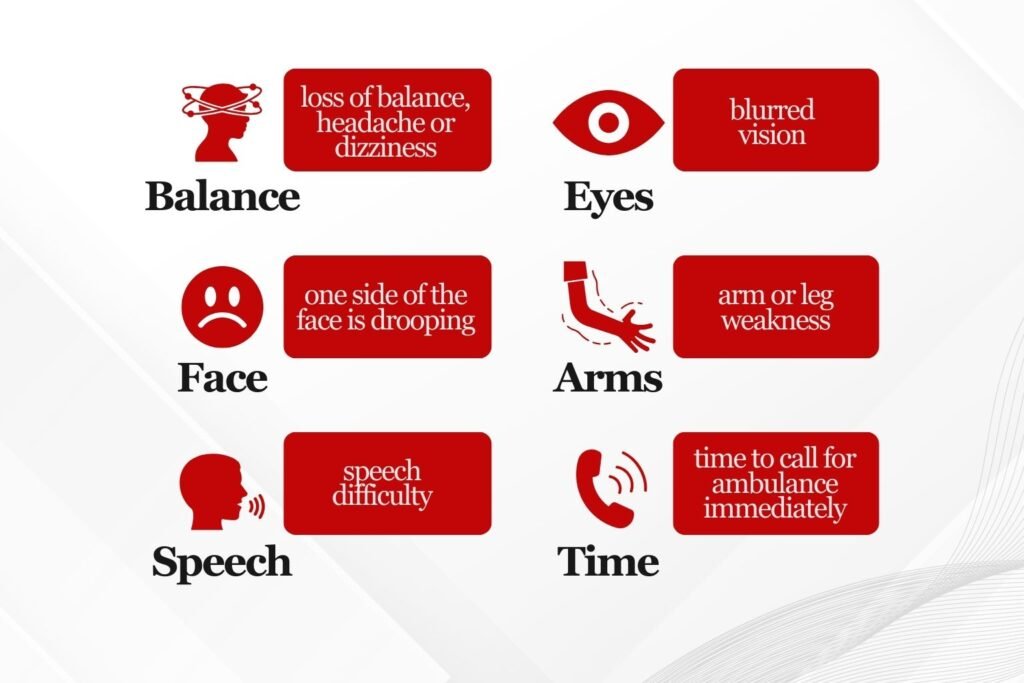
Early recognition of stroke symptoms is critical. The FAST method is commonly used:
Face drooping, Arm weakness, Speech difficulty, Time to call emergency services.
Additional warning signs include sudden confusion, vision loss, difficulty walking, severe headache, or dizziness without an obvious cause.
This section addresses emergency response, not prevention. If symptoms occur, seek immediate medical care.
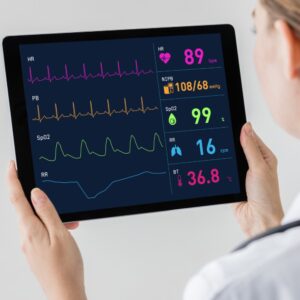
The Role of Monitoring in Long-Term Brain Health
Monitoring physiological markers such as blood pressure, heart rhythm, and oxygen levels can help identify trends that warrant clinical evaluation. Over time, pattern recognition may support more informed medical decision-making.
Monitoring alone does not prevent stroke. Its value lies in supporting earlier intervention when abnormalities are detected.
Stroke Prevention Technology — What It Can and Cannot Do

Digital health tools and monitoring technologies can assist with data collection and long-term trend awareness. They may say identify changes that prompt clinical review.
These tools do not diagnose disease, prescribe treatment, or replace medical care. Clinical evaluation remains essential for stroke risk assessment and management.
Technology supports care. It does not replace it.
Wearables and Heart–Brain Signals: An Emerging Area

The relationship between cardiovascular physiology and neurological health is an active area of research. Wearable devices are being studied for their ability to observe patterns that may correlate with long-term brain health.
Current evidence supports continued investigation. These tools are not substitutes for clinical evaluation or preventive treatment.
When to Talk to a Clinician About Stroke Risk

Consider speaking with a healthcare professional if you have high blood pressure, a history of transient ischemic attack (TIA), atrial fibrillation, diabetes, difficulty controlling cardiovascular risk factors, or a family history of stroke.
Early clinical guidance allows for individualized risk assessment and appropriate preventive planning.